A bridge is a device that is used as one of the ways of replacing a missing tooth.
There are two types of bridge; a conventional bridge or an adhesive bridge.
-
Conventional bridge
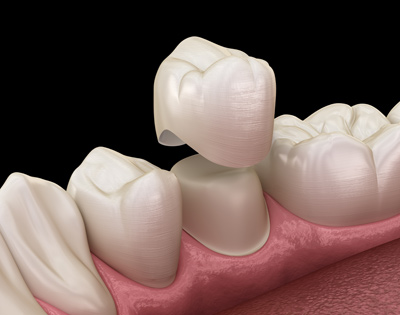
A false tooth is attached to a crown on one or both sides of a gap. It involves quite extensive drilling of the tooth (or teeth) to which the false tooth will be attached. The crowns are either made of gold, a non-precious metal, or a combination of metal and porcelain. The false tooth is usually made out of tooth-coloured porcelain.
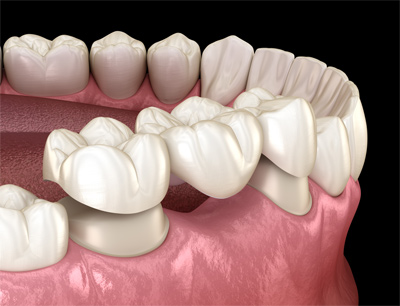
Once the teeth have been prepared, a mould (impression) of the affected teeth is made. This is sent to a laboratory for the bridge to be made; it usually takes two weeks. In the meantime, to prevent any sensitivity, a temporary bridge covers the drilled teeth.
Once it has been manufactured, the bridge will be tried in place. It may require some adjustments before it is cemented in permanently.
The advantages of a conventional bridge are that it is strong and not removable. The disadvantage is that it involves extensive drilling of the adjacent teeth.
-
Adhesive bridge
A false tooth is attached to a wing of metal and the wing is then glued to the adjacent tooth.With this type of bridge there is no (or only a small amount of) drilling of the adjacent teeth. An injection is normally not required. Once the teeth have been prepared, a mould is made and sent to a laboratory which makes the bridge. The bridge usually takes two weeks to make. No temporary bridge is required.
When using an adhesive bridge to replace a front tooth, the metal wing is stuck on to the back of the adjacent tooth and so cannot be seen from the front. An adhesive bridge replacing a back tooth will have metal wings on one or both sides of the gap. These may be visible if the mouth is opened wide.
The adhesive bridge is stuck on with a very strong glue. The process requires that the teeth be dry whilst gluing.
The advantages of an adhesive bridge are that it is not removable and requires very little drilling of the adjacent teeth. The disadvantage is that it sometimes falls off (though it is easily stuck back on). An adhesive bridge might not be suitable for those who grind their teeth or who play contact sports.
A bridge is not always possible or suitable, for example if there are too many teeth missing or if the remaining teeth or gums are not healthy. In some instances, it may be best to leave a gap.
Alternative treatments to bridges include removable dentures (false teeth) or dental implants (screw-in teeth).


















 Fantastic service and results from David and the team, I had two porcelain front crowns fitted and the shading match to my own teeth was perfect. David is very relaxed and takes time to consider all options available and puts you totally at ease
Fantastic service and results from David and the team, I had two porcelain front crowns fitted and the shading match to my own teeth was perfect. David is very relaxed and takes time to consider all options available and puts you totally at ease